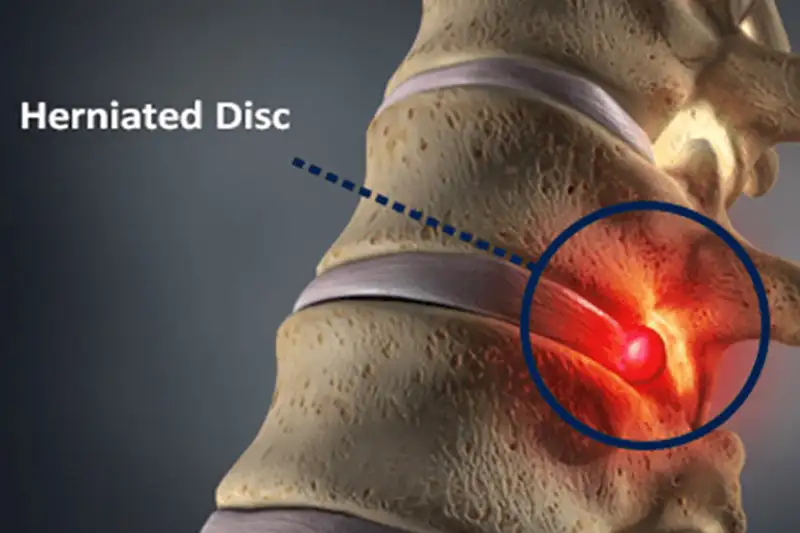
What is a Herniated Disc?
A herniated disc occurs when one of the discs located between the vertebrae in the spine gets damaged. These discs act as shock absorbers and keep the vertebrae from rubbing against each other. There are several terms used to describe disc pathology, including herniated disc, bulging disc, and pinched nerve.
Their symptoms are often similar. Medical professionals do not always agree on their definitions, frustrating patients trying to get a medical diagnosis. Adding to the confusion are an unusually wide range of terms also used to describe spinal disc problems, including slipped disc, ruptured disc, torn disc, collapsed disc, disc disease, disc protrusion, and black disc.
The discs become less elastic with age and more vulnerable to injury. As the discs become less elastic, they can rupture due to stress on the body.
When a disc ruptures, a portion of the spinal disc pushes outside its normal boundary. When a disc bulges out, it pinches the spinal nerves that are located very close to the disc. Therefore, the spinal nerves and spinal cord can become compressed causing pain, numbness, weakness and other herniated disc symptoms.
There is normally enough extra space around the spinal cord and spinal nerves. However these structures become compressed if too much of the herniated disc is bulging. When you have a symptomatic herniated disc, it is the not the disc itself that is painful, but the pain caused by the disc pinching the nerve that causes you to feel pain. A herniated disc is also often referred to as a slipped disc.
What Causes Herniated Discs?
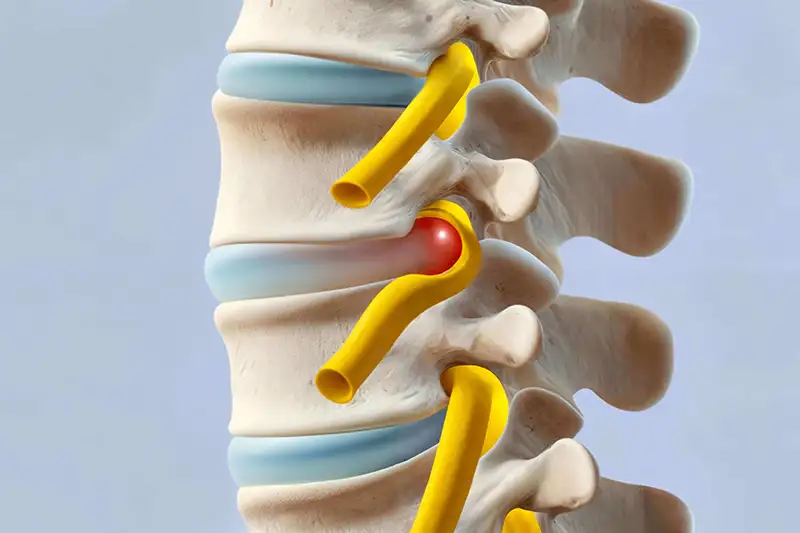
Most herniated disc causes are from the gradual age-related wear and tear on the spine, called disc degeneration. Spinal discs lose some of their water content due to age. That makes them more likely to tear or rupture.
Most patients can’t pin down exactly what caused their herniated disc. Some causes include using your back muscle instead of your leg muscles when lifting heavy objects, twisting or turning while lifting, and rarely, a traumatic event such as a blow to the back or a fall.
Disc herniation occurs more frequently in middle-aged and older people, especially those involved in strenuous physical activity. Symptoms of a herniated disc may also be caused by trauma of some sort such as a car accident or lifting something heavy which may require treatment.
Generally common causes of a herniated disc include:
- Aging and general degeneration of the intervertebral discs
- Trauma related to automobile accidents
- Sports injuries
- Improper or heavy lifting
A bulging disc is often the beginning stage of a herniated disc.
Signs & Symptoms of a Herniated Disc
A herniated disc is a fairly common condition. As discs degenerate, the inner material in the disc can leak into the spinal canal. This is a condition known as a herniated disc or disc herniation. When the inner material of the herniated disc reaches the spinal canal, the material puts additional pressure on disc is what is referred to as disc herniation or herniated disc.
Herniated Disc Locations
As with many spine conditions, a herniated disc can occur along the spine. However, the most common location is the lumbar region or lower back. This is due to the constant impact this area bears, especially when standing or sitting.
A herniated disc can occur in the:
- Cervical spine (neck) – C1 through C7 vertebrae
- Thoracic spine (upper back) – T1 through T12 vertebrae
- Lumbar spine (lower back) – L1 through L5 vertebrae
The location of the herniated disc will determine the symptoms someone will experience. Most symptoms include pain, weakness, and numbness. In some extreme cases, a restricted range of motion can also be experienced. However, these symptoms will vary according to the location.
Lumbar Herniated Disc Symptoms
The lower back is the most common location for herniated discs. Because the lower back serves as a primary shock absorber and supports the upper body, spinal discs in this area tend to wear down faster. Some of the common symptoms associated with lumbar herniated discs include:
- Leg pain that radiates along sciatica.
- Sharp, radiating, electric, and piercing pain spasms in the legs.
- Pain that radiates to the buttocks, thigh, calf, or foot.
- Difficulty lifting the foot when standing or walking.
- Lower back pain that is described as throbbing or dull, with stiffness.
- Pain that worsens with movement or hunching forward.
Thoracic Herniated Disc Symptoms
Although thoracic herniated discs are less common, it often occurs at the mid back. Most thoracic spine conditions are asymptomatic, which is why most people live with a herniated disc in this area without notice. Herniated disc in the thoracic spine can occur in central, lateral, or centre-lateral directions. These are the most common symptoms:
- Upper back pain.
- Pain that radiates to the chest wall or abdomen.
- Radiating pain that reaches the upper back.
- Myelopathy or spinal cord dysfunction.
Cervical Herniated Disc Symptoms
Because the space in the cervical spine is limited, even the smallest herniation can impinge on adjacent nerves causing significant pain. Symptoms from a cervical herniated disc are often experienced in the arms, neck, hands, and fingers, as well as sections of the shoulders. Symptoms will also vary according to the nearby vertebrae affected. The most common symptoms include:
- Shoulder pain and weakness in the upper arm.
- Weakness in the biceps and numbness or tingling that can radiate to the thumb side of the hand.
- Numbness, weakness, and tingling along the triceps into the middle finger.
- Difficulty or weakness with handgrip and pain that radiates to the little finger side of the hand.
Herniated disc symptoms are often confused with other conditions such as pinched nerves, sciatica, or frequent neck pain. This is why discussing all symptoms with a physician can help those experiencing similar symptoms pin point their condition and discuss possible treatment options.
Get Expert Herniated Disc Treatment in Tampa Bay
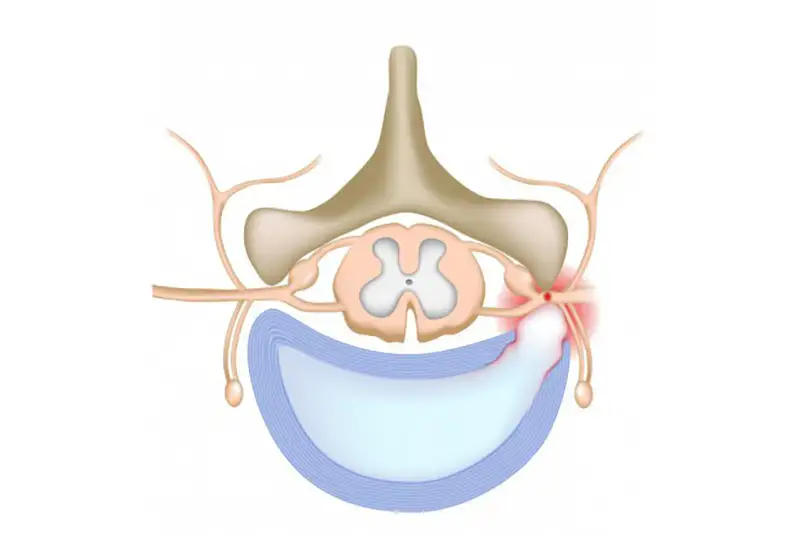
The Bonati surgery for a herniated disc is a safe and effective solution to treat lumbar, thoracic and herniated discs in the neck, that have not responded to conservative treatment. Severely herniated discs may not heal on their own and require surgical intervention.
The Bonati Spine Procedures are extremely effective at fixing the problem, resolving the symptoms and returning the patient to normal, pain-free activities within days of surgery. These procedures are performed on an out-patient basis, with the patient under local anesthesia and twilight sedation. These techniques allow our our experienced team of spine surgeons to utilize the patient as a monitor and determine that the surgery has been successful even prior to the patient leaving the surgical room. The patients walk-out on their own, within a couple of hours of their surgery and most are able to return to work within days. These highly effective revolutionary outpatient surgeries are designed to address the problem, fix it and provide immediate relief for the symptoms caused by herniated discs.
The Bonati Spine Procedures may utilize an array of surgical procedures to treat herniated discs. These procedures may include:
Discectomy for a Herniated Disc
A discectomy is a surgical procedure performed to remove a portion of the bulged or herniated disc, thereby relieving pressure on the impacted spinal nerves or spinal cord. The Bonati surgery for herniated discs involves a very small incision through which the patented Bonati tube system is inserted to provide the surgeon with direct visualization. Surgical instruments are passed through the tubular system to remove small portions of tissue to provide access to the portion of the disc that is compressing the nerve root or spinal cord. The Bonati Discectomy is performed using local anesthesia and Conscious IV Sedation, allowing the patient to be comfortable and responsive during the procedure.
Foraminotomy for a Herniated Disc
A foraminotomy is a decompression surgery performed in order to increases the space of the foramen and hollow out the passageway where the nerve roots exit the spinal canal. The procedure involves the removal of bone or tissue that obstructs the neuroforamen and compresses the nerve roots leading to inflammation and radiating pain. The removal of part of the lamina is often necessary for the surgeon to gain access to the affected nerve roots in the neuroforamen or to a herniated disc. For this reason the foraminotomy is often performed in conjunction with a laminectomy or laminotomy.
Laminectomy for a Herniated Disc
A laminectomy is a surgical procedure performed to relieve pressure (decompress) on the spinal cord or spinal nerve roots through the widening of the spinal canal. The procedure is carried out by removing or trimming part of the lamina (roof) of the vertebrae in the affected area. The removal of part of the lamina creates an opening for the compressed nerves, relieving pressure on the nerve roots and reducing inflammation. The partial removal of the lamina also allows the surgeon access to a herniated disc to remove any tissue causing pain and inflammation.
Laminotomy for a Herniated Disc
A laminotomy is a common decompression surgery for spinal stenosis that resembles the laminectomy in its goals and technique. The difference between the laminectomy and the laminotomy is that the laminotomy involves making an opening in the lamina to gain access to the disc, where the laminectomy necessitates the partial removal of the lamina. In either case, the goal is similar, to relieve pressure on the affected area and allow the nerve roots room to heal. Both procedures are often utilized in order to give the surgeon the proper space to perform a foraminotomy or discectomy.
The Bonati Spine Institute encourages patients with a herniated disc to contact us to request a no-obligation MRI review or discuss your conditions with our medical professionals. Find out why The Bonati Spine Procedures are considered to be among the world’s best solutions when it comes to advanced spine surgery. Your pain from disc herniation can become a thing of the past.
Ruptured Disc
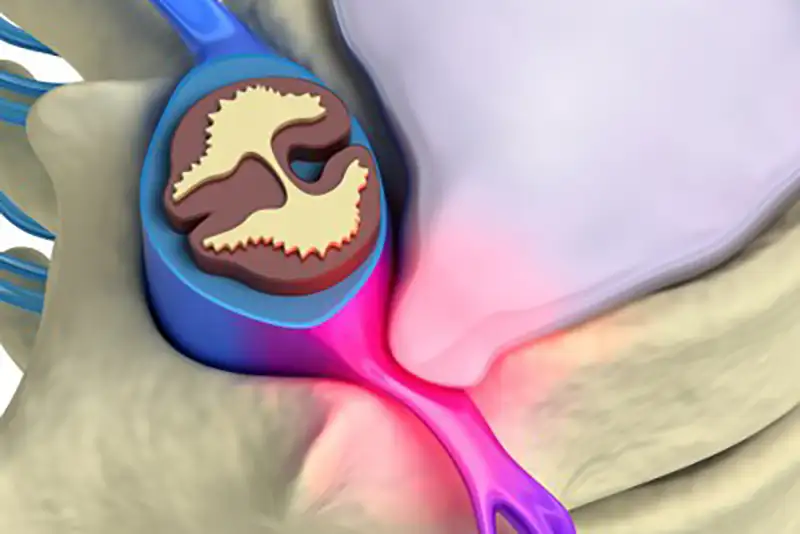
A ruptured disc, sometimes referred to as a herniated disc, is a common condition that can result in pain and discomfort.
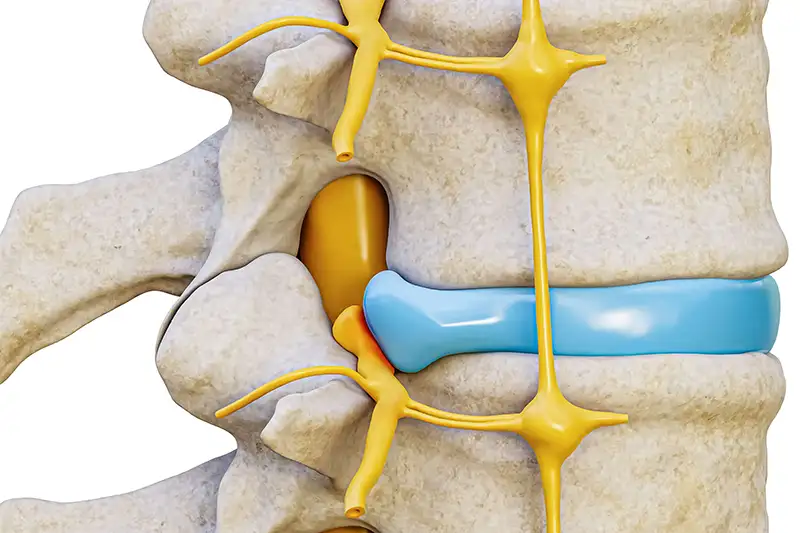
Intervertebral discs, located between spinal vertebrae, act as small cushions that protect the spinal column as it moves and bends. These discs act as shock absorbers that protect the spine from everyday stress. When a ruptured disc occurs, gel-like material from the nucleus pulposus, located at the core of the vertebral disc is released into the spinal canal, causing the nerves to be compressed. Numbness or tingling may result once the disc starts compressing a spinal nerve.
The spine has 24 moveable bones called vertebrae. Each vertebra is separated by discs, which act as shock absorbers preventing the vertebrae from rubbing together. The outer wall is called the annulus fibrosus. Each disc has a gel-filled center called the nucleus pulposus. At each disc, a pair of spinal nerves exits the spinal cord and branches out to your body, allowing messages or impulses to travel back and forth between your brain and your body.
What is a Ruptured Disc
A ruptured disc occurs when the gel-like center of your disc ruptures out through a tear in the disc wall. This irritates the nerves and causes inflammation and swelling.
A ruptured disc can occur in any part of the spine. The more common are on the lower back (lumbar spine), or in the neck (cervical spine). Ruptures in the thoracic region can occur, though are rarer since the thoracic spine is less mobile. Due to the disc’s displacement, the disc presses on spinal nerves, often producing pain.
Causes of a Ruptured Disc
In many cases, a ruptured disc develops due to wear and tear. A single strain or injury can cause a ruptured disc. However, aging plays a big role. Disc material degenerates naturally as we age, which is why a relatively minor strain or movement can cause a disc to rupture. Genetics, smoking, and a number of occupational and recreational activities lead to early disc degeneration.
A ruptured disc can also arise from spinal stenosis, which is when your spinal canal starts to narrow as part of the natural aging process. This usually occurs in adults 50 and older, leading to pain and other problems. Also, patients with a congenital spinal deformity are prone to a ruptured disc, since their malformation creates pressure on different points throughout the spine that can cause a ruptured disc.
The loss of fluid in your disc may often cause degenerative disc disease, which is the term used to describe the normal changes in your spinal discs as you age. Degenerative disc disease causes your discs to become softer, which can cause a ruptured disc.
Sudden injury, such as those that occur in a car accident, high-impact sports, or a hard fall can also cause a ruptured disc. On the other hand, lack of regular exercise can also cause weakening of the spine, as well as, malnutrition, obesity, and the excessive use of alcohol.
Symptoms of a Ruptured Disc
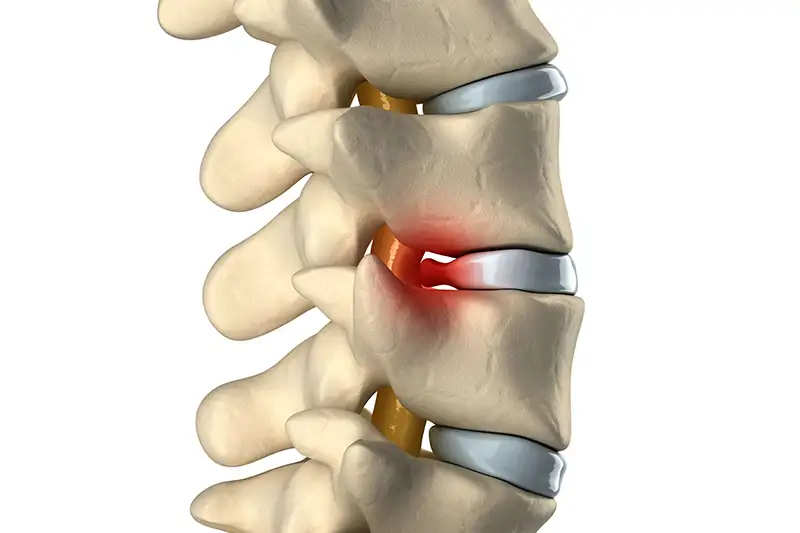
Symptoms can differ from patient to patient. Usually individuals notice changes when the displaced disc begins to aggravate surrounding components of the body creating nerve pain.
Some of the symptoms many experience are:
- Spasms
- Muscle tightness
- Tingling
- Weakness in the affected area
- Pain that goes through the shoulders, arms or down the legs
Because some of these symptoms mirror other spine conditions, it is important to get a comprehensive diagnosis.
In some rare cases, a ruptured disc can start compressing the spinal cord itself, in which case can be very dangerous and should be handled as an emergency.
Diagnosis
Diagnosis is made by a neurosurgeon based on symptoms, history, physical examination, and imaging studies. After reviewing your medical history, your doctor evaluates your current symptoms and what makes them better or worse. Further examination determines how severe the condition is. The different tests can offer more information on locating the rupture, assess the degree of the rupture, and confirm the diagnosis.
Exams & Tests
After a primary diagnosis has been made, different exams and tests will confirm the diagnosis, including:
- X-ray: X-rays of the spine are obtained to find other potential causes of pain like tumors, infections, fractures, etc.
- CT scan: A computed tomography scan shows the shape and size of the spinal canal, its contents, and the structures around it.
- MRI: This test produces a 3-D image of your body structure which shows the spinal cord, nerve roots, and surrounding areas.
- Myelogram: A contrast injection into the surrounding cerebrospinal fluid spaces shows where there is pressure on the spinal cord or nerves due to a ruptured disc, bone spurs or tumors.
Treatment for a Ruptured Disc
Many patients find relief with conservative non-surgical treatment. However, if your body doesn’t respond to conservative treatment or your symptoms worsen, a surgical intervention may be required.
Non-Surgical Treatment
In most cases, the pain will get better within a couple of days and completely resolve within 4 to 6 weeks. Ice/heat therapy, and taking over the counter medications can help with recovery. Most common non-surgical treatments include:
- Prescribed medication
- Physical therapy
- Holistic therapy
- Epidural injections of cortisone
- Hot/Cold therapy
- Laser therapy
- Ultrasound therapy
Surgical Treatment
When symptoms progress rapidly or your body is non-responsive to treatment, surgery may be required. There are a lot of factors to consider before choosing a surgical intervention, such as age, the severity of the problem, other medical problems, and other spine interventions. If surgery is recommended, your doctor may perform any of the following surgical approaches:
- Foraminotomy
- Laminectomy/Laminotomy
- Discectomy
- Partial Pediculectomy
Prevention & Self-Care
After the patient has recovered from surgery and with the doctor’s approval, moderate exercise may be resumed. However, prevention and self-care are crucial to keep and enhance your spine health. Consider implementing the following recommendations:
- Moderate regular exercise
- Use correct lifting and moving techniques
- Maintain correct posture
- Avoid smoking
- Avoid stressful situations
- Maintain a healthy weight
Prolapsed Disc
A prolapsed disc is also called a slipped disc. But no matter what you call it, it often causes severe lower back pain.
Bouts of back pain are very common, in fact, 31 million people experience low back pain at any given time. While this back pain is sometimes caused by a minor problem in a muscle, ligament, or other structure in the back, it can also be caused by a prolapsed disc. Twice as many men than women develop a prolapsed or slipped disc and the condition generally arises between the ages of 30 and 50.
When a prolapsed or slipped disc puts pressure on a nerve root, it can cause pain and other symptoms in the extremities innervated by the compressed nerve root. Sometimes, the symptoms resolve in several weeks on their own, but often they linger for more than 6 weeks. If the symptoms persist and become either acute or chronic, surgery may be an option.
Anatomy
The spine consists of many small bones called vertebrae. The spine has 33 vertebrae: 7 cervical, 12 thoracic, 5 lumbar, 5 fused sacral vertebrae, and 4 often fused coccygeal vertebrae.
Between each of the 24 presacral vertebrae (cervical, thoracic, and lumbar) there is an intervertebral disc made up of strong rubber-like material (annulus fibrosus). Each intervertebral disc has a soft, jelly-like interior called the nucleus pulposus surrounded by a strong outer ring of fibrous tissue. The discs cushion the vertebrae and allow the spine to be flexible.
The spine houses the spinal cord, which is composed of the nerves that come from the brain and then branch out between the vertebrae to pass messages to and from the brain to various parts of the body, including the extremities.
Strong ligaments attached to the vertebrae provide extra strength and support to the spine, thus further protecting the spinal cord. In addition, various muscles are also attached to, and surround, the spine.
What Is a Prolapsed Disc?
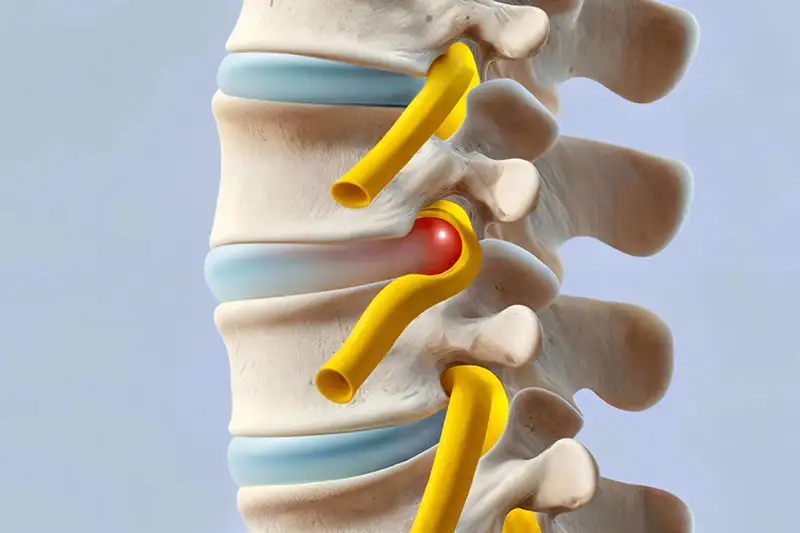
Although a prolapsed disc is often referred to as a “slipped” disc, this is a misnomer. The disc doesn’t actually slip. What occurs is that the nucleus pulposus – the soft inner center of the disc – pushes or bulges out through a weakness in the fibrous outer part of the disc. This is also often called a herniated disc.
When the prolapsed disc presses on nearby structures of the spine, such as a nerve exiting the spinal cord, it can cause back pain and other symptoms. The sciatic nerve is the most commonly affected nerve. Usually, inflammation develops around the prolapsed disc, which can also cause back pain.
Where Does It Occur?
A disc prolapse can occur in any of the 24 presacral vertebrae in the spine. However, a disc prolapse is most likely to occur in the lumbar spine (lower back). In general, the larger the prolapse, the more severe and painful the symptoms.
Cervical Prolapsed Disc
Although disc prolapse is more common in the lower back, it can occur in the 7 vertebrae of the cervical spine. Levels C4 to C7 of the cervical spine are the most vulnerable to disc prolapse.
Lumbar Prolapsed Disc
Prolapsed lumbar discs are by far the most common. This condition is also sometimes called a ruptured, herniated, or slipped disc. It is most often caused by age-related deterioration in the spine. A prolapsed disc can happen at any age but becomes more likely after the age of 35.
Thoracic Prolapsed Disc
Since the thoracic spine is the least mobile portion of the spine, it is the least common area for a prolapsed disc to occur. The symptoms of a thoracic prolapsed disc vary depending on where the prolapsed disc occurs. The prolapsed disc can impinge on either a nerve, nerve root or on the spinal cord itself. It can herniate in a central, lateral, or centro-lateral direction.
Causes of a Prolapsed Disc
Many things can trigger the nucleus pulposus to prolapse out through a weakness in the outer fibrous ring of a disc. Awkward bending, poor mechanics when lifting heavy items, or even sneezing may be enough to cause a disc prolapse in people who have a weakness in a disc.
Risk factors for developing a prolapsed disc include:
- Trauma that causes the vertebra to fracture
- A job that requires lots of lifting
- A job that requires a lot of sitting
- Weight-bearing sports or exercise
- Obesity
- Smoking
- Weight-bearing sports or exercise
- Weakness in the spine due to normal aging
Symptoms of a Prolapsed Disc
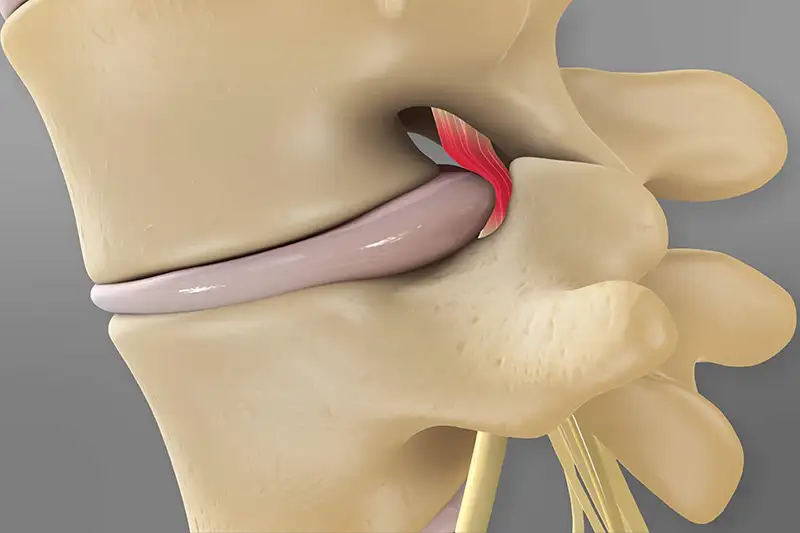
The symptoms of a prolapsed disc are generally specific to the area of the spine in which the prolapse has occurred. Although the symptoms may not include neck or back pain in some patients, such pain is common. The main symptoms are listed below.
- Numbness, tingling, or pins and needles in the extremities
- Pain in the buttocks or behind the shoulder blades
- Pain radiating down one or both arms or legs
- Weakness involving one or both arms or legs
Symptoms in severe cases may include loss of bowel or bladder control, numbness in the genital area, and impotence.
Cauda Equina Syndrome
Although rare, cauda equina syndrome is a serious nerve root problem that can be caused by a prolapsed disc. The nerves at the very bottom of the spinal cord become compressed. In addition to low back pain, the condition causes:
- Bowel and bladder control problems and function (inability to pass urine).
- Numbness in the saddle area around the back passage (anus).
- Weakness in one or both legs.
This syndrome is considered an emergency and requires urgent treatment to avoid permanent damage to the nerves in the bowel and bladder. If you develop these symptoms, see a doctor immediately.
Diagnosis
Your physician will begin with an assessment of your physical condition and review of your medical history. In some cases, no tests are needed and the symptoms will disappear in a few weeks. However, imaging tests such as x-rays, CT-scans, or MRIs might be required if your symptoms persist or are severe. These imaging studies can show the level of the spine where the disc is prolapsed and will be needed if your doctor recommends surgery.
Exams & Tests
Depending on your symptoms, your doctor may require one or more of the following tests during the physical exam:
- Nerve function in certain parts of the leg or arm
- Muscle strength
- Pain with motion or palpitation
After the physical exam, a diagnostic imaging test or tests may be ordered to rule out some conditions, confirm the diagnosis, or gather more information.
These tests include:
- X-ray to rule out other conditions as the source of the symptoms
- CT scan to better visualize the affected disc and surrounding area
- MRI scan for an accurate assessment of the spinal nerves and anatomy
- Discogram to confirm which disc is causing the symptoms. This test is controversial and not all doctors use it.
Treatment for a Prolapsed Disc
Many people opt for non-surgical treatment for a prolapsed disc. Everyone is different and not all treatments work for all patients. If you are still suffering from acute or chronic pain that negatively impacts your daily life, surgery may be necessary.
Non-Surgical Treatment
Continue with your normal activities unless your pain is severe. In the past, resting until the pain subsided was recommended but we now know you are likely to recover faster if you stay active. Staying active also lowers your chances of developing chronic back pain. However, a general rule is to refrain from activities that cause severe pain.
Non-surgical treatment for a prolapsed disc may include:
- Moderate, low-impact exercise to strengthen the surrounding muscles
- Physical therapy, including massage, stretching, and thermotherapy
- Alternative treatments such as acupuncture
- Painkillers such as paracetamol or codeine
- Anti-inflammatory painkillers such as ibuprofen, naproxen, or diclofenac
- Muscle relaxants such as diazepam or carisoprodol
Surgical Treatment
If you have tried non-surgical treatment options and are still in pain, surgery may be necessary.
The Bonati Spine Institute offers an array of procedures to treat disc problems. These procedures may include:
- Foraminotomy/Foraminectomy
- Laminotomy/Laminectomy
- Discectomy
Prevention & Self-Care
Preventing a prolapsed disc requires avoiding behaviors that may lead to intervertebral disc degeneration. Some things can’t be avoided, such as degenerative disc disease due to normal aging. But there are ways to strengthen the neck and back as well as reduce deterioration of the spine.
- Maintain a healthy weight
- Exercise regularly
- Stretch correctly
- Improve posture while standing, sitting, and sleeping
- Avoid excess alcohol consumption
- Quit smoking
- Use proper lifting techniques
Slipped Disc
Nerves extend from your brain through the spinal cord and relay important messages between the body and the brain. When you have a slipped disc and that disc is causing a nerve to be compressed or pinched, your body may send warning signals such as pain. If not diagnosed and promptly treated, that pain can become chronic and impact your quality of life.
Anatomy
The spinal cord runs from the base of the brain, through the cervical and thoracic spine and exits at the lumbar spine. The nerve roots at the lumbar and sacral levels exit the spinal canal in a horse’s tail formation. There are 33 stacked, interlocking spinal vertebrae that make up the spinal column and house the spinal canal.
Between each vertebra is an intervertebral disc that acts as a shock absorber and cushions the spine. Each disc has a soft center, the nucleus pulposus, composed of a gelatinous substance, and hard outer ring, the annulus fibrosus. It is the discs’ cushioning of the vertebrae that allows the spine to flex and bend without pain.
What Is a Slipped Disc?
Also known as a herniated disc or bulging disc, a slipped disc occurs when one or more disc has “slipped” out of place. An injury or weakness in the disc can cause the inner nucleus pulposus to protrude through the outer annulus fibrosus. While some slipped discs go unnoticed, when one compresses a spinal nerve, or nerve root root, they cause pain and discomfort.
Causes of a Slipped Disc
A slipped disc occurs if the annulus fibrosus becomes weakened and the nucleus pulposus slips out. It is most often the result of age-related wear-and-tear on the spine. As you age, the nucleus pulposus loses some of its water content, making the disc less flexible and more prone to tearing. Although a part of the normal aging process, there are some instances in which a ruptured disc is more likely to happen, such as:
- Improperly lifting heavy objects
- Obesity
- Trauma or injury to the spine
- Physically demanding work
- High-impact sports
- Osteoarthritis or rheumatoid arthritis
Symptoms of a Slipped Disc
A slipped or herniated disc can occur at any level of your spine. The lumbar spine is the most common area for a slipped disc. A slipped disc can put pressure on the nerves and muscles that surround it, causing pain and other symptoms such as:
- Numbness and pain, usually on one side of the body
- Pain that radiates through the arms and legs, depending on the level of the torn disc
- Pain intensifies with certain movements or at night
- Pain intensifies after standing or sitting
- Pain that occurs when walking short distances
- Burning, tingling, or aching sensations in the affected area
- Unexplained muscle weakness
Diagnosing a Slipped Disc
See your doctor if the signs and symptoms of a slipped disc last for more than a few weeks and don’t respond to rest and over-the-counter pain relievers and the symptoms are impacting your quality of life. Your physician will review your medical history, take a complete inventory of your symptoms, and examine your back for tenderness.
Exams & Tests
During the physical exam, your doctor may also perform a neurological exam to check your muscle strength, reflexes, balance, walking ability, and the ability to feel vibration, pinpricks, and light touches.
Your doctor may order imaging studies to rule out other possible causes for your slipped disc and confirm the diagnosis. These tests include:
- X-rays to rule out the possibility of infection, tumor, broken bones, or spinal alignment issue
- CT scan to better visualize your spine and the structures around it
- MRI to confirm the location of the herniated disc and the nerves affected by it
- Myelogram to determine the pressure on your spinal cord or nerves due to multiple herniated discs or other conditions
Risk Factors
While normal age-related generation of the spine is the main cause of a slipped disc, there are risk factors that may increase their occurrence, such as:
- Obesity as excess weight puts additional stress on your spine
- Occupations that are physically demanding and require repetitive lifting, pushing, pulling, bending and twisting
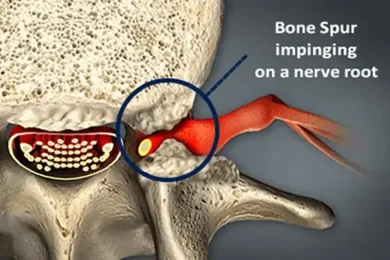
- Bone spurs that develop when two bones rub against each other and cause narrowing of the spine
- Smoking can speed up disc degeneration and slow down healing
- Hereditary tendency of disc degeneration that can increase the risk of a slipped disc
Treatment for a Slipped Disc
Most physicians begin with conventional, non-surgical treatments to provide pain relief for their patients suffering from a slipped disc. Often, avoiding painful positions and movements as well as an exercise regimen and pain medication relieves symptoms within a few weeks.
Non-Surgical Treatment
Non-surgical treatments for a slipped disc include:
- Over-the-counter pain medication such as ibuprofen, naproxen, or acetaminophen
- Muscle relaxers for patients who have had muscle spasms
- Non-steroidal anti-inflammatory drugs (NSAIDs) to reduce inflammation and provide pain relief
- Cortisone injections into the area around the spinal nerves
- Oral steroids to reduce swelling and inflammation
- Physical therapy
- Alternative methods such a chiropractic care or acupuncture
Surgical Treatment
If your symptoms have not subsided and your pain has worsened to the point that it is chronic and impacting your quality of life, surgery may be necessary. The Bonati Spine Institute offers an array of procedures to treat a slipped disc, which may include:
Surgeries for a slipped disc include:
- Foraminotomy/Foraminectomy to increase the space in the foramen and decompress the nerve root
- Laminectomy/Laminotomy to relieve pressure on the spinal cord by removing a section of the lamina
- Discectomy to remove a portion of the disc that is compressing the nerve roots
Slipped Disc Surgery
Surgery for a slipped disc is necessary when conservative treatment options has failed to relieve symptoms such as pain in the back or neck, or pain that radiates to the arms or legs. A slipped disc occurs when the soft gel-like tissue between the bones of the spine is moved out of place and starts pressing on adjacent nerves. In most cases, slipped discs are caused by wear and tear or trauma to the spine.
This condition is also known as herniated disc, ruptured disc, or prolapsed disc. The most common affected area is the lower back, but many discs along the spine can slip, including those in the neck. While the majority of cases don’t call for surgery, severe cases or when there is evidence of muscle malfunction, surgery may be needed.
When Is Slipped Disc Surgery Done
In many cases, slipped discs can get better with conservative treatment and time. If conservative treatment is not effective, spine surgery may be necessary. Surgery may also be a viable option if symptoms like lower back pain, numbness in shoulders, arms, or legs, unexpected muscle weakness, and problems bending or twisting your back are severe or worsen over time.
Slipped disc surgery may involve the removal of the portion of the disc pressing on the nerves or nerve roots, along with other procedures.
Traditional Open Back Surgery and Spinal Fusion for Slipped Disc
“Open” spine surgery is the traditional surgical approach to treating a slipped disc. There are many disadvantages and risks associated with this type of procedure. In this approach, a surgeon creates space by removing the part of the vertebra- that lamina- that covers your spinal canal and/or part of the disc. This procedure enlarges the spinal canal and relieves pressure on the spinal cord and the nerves that pass through it. Traditional open spine surgery has a long recuperation time due to extensive dissection of muscles and tissues to access the area.
Spinal fusion surgeries use bone grafts and/or hardware to permanently “lock” together two or more vertebrae for the purpose of making a section of the spine thought to be producing pain symptoms immobile. After a fusion surgery, the patient will likely lose the ability to move his/her spine at the level where the procedure was done. This puts extra pressure on adjacent vertebrae, forcing the intervertebral discs to breakdown, which can lead to a condition known as adjacent segment disease.
Traditional open back surgery and spinal fusions often require an extensive dissection of muscle tissue, several days of hospitalization, and an often painful and long recovery. Failed back surgery syndrome is common in traditional open back surgery and spinal fusions with about 60% of patients experiencing failed back surgery symptoms.
The Bonati Spine Institute strongly recommends against open spine surgery and spinal fusions and implants, since these procedures result in high failure rates.
The Bonati Spine Procedures for Slipped Disc
The Bonati Spine Procedures are safe and effective alternatives to traditional open back surgery and spinal fusions. The Bonati Spine Procedures have been shown to be highly effective in decompressing the nerves without fusions to treat spinal conditions and very successful in avoiding adjacent segments disease.
The Bonati Spine Procedures do not require general anesthesia. Using conscious IV sedation and local anesthesia, the patient is comfortable, and responsive and maintains the ability to provide feedback to the surgeons throughout the procedure. The procedures are outpatient and no hospital stay is necessary. There is a short recovery time and patients are able to get back to their normal daily activities within days.
The goal of slipped disc surgery is to alleviate the pain and resolve the underlying problem. The Bonati Spine Institute offers an array of procedures to treat a slipped disc, which may include:
Discectomy
This is perhaps the most common surgical approach to treat slipped discs. A small incision is made and a series of tubes are inserted to view the surgical area using endoscopic assistance. A portion of the herniated disc is removed to release pressure from the spinal nerves and/or spinal nerve roots.
Laminectomy/Laminotomy
A laminectomy is a decompressing surgery that relieves pressure on the spinal nerves. This procedure is performed one vertebral level at a time, to address the primary cause of the pain first. A laminectomy is performed through a small opening through which a series of tubes are introduced to accommodate surgical tools and imaging equipment. The lamina is then accessed through an arthroscope, and small portions of the lamina are removed to release the pressure from the spinal nerves.
Foraminectomy
Foramina are small openings present between every pair of vertebrae in the spine. If a part of the foramen is pressing on a nerve as it leaves the vertebral opening, a Foraminectomy may be performed. This procedure uses local anesthesia and conscious IV sedation to allow surgeons to target the source of the pain with precise accuracy. The tissue compressing the nerves is removed with a set of surgical instruments inserted through a very small incision.
Before Surgery
It is important to be in your best physical and mental health possible before a surgery. To assure this, maintain a healthy diet and exercise routine. Before any surgery, you may be asked to stop taking certain medications, and stop smoking. Medications to avoid include:
- Advil
- Anaprox
- Coricidin
- Aspirin
- Excedrin
- Ibuprofen
- Naprosyn
- Voltaren
Make sure you have a companion who can drive you and stay during the surgery and the first night. Pack loose-fitting, comfortable clothing, preferably something that can be zipped or buttoned.
During Surgery
During surgery general anesthesia is not used, instead, local anesthesia and conscious IV sedation are used by the surgical team. With this approach, the patient is responsive, comfortable, and able to provide feedback to the doctors throughout the procedure without feeling any pain or discomfort. While in the operating room, the surgical team will confirm the patient is able to complete a series of mobility exercises and verify that the pain has been successfully treated.
After Surgery
After the procedure, the patient is transferred to postoperative care for rest and observation. Later on a postoperative consultation will determine if additional procedures are necessary. During this time, most patients are given a walking regimen schedule to start the healing process.
Recovery Time from Slipped Disc Surgery
Recovery time after slipped disc surgery varies from patient to patient. Every patient, every slipped disc, every circumstance is different. The Bonati Spine Procedures allow for faster recovery so most patients resume their everyday life within days.
The success rate for slipped disc surgery is generally high. Patented Bonati Spine Procedures have a 98.75% patient satisfaction rate. Our procedures offer a lower risk of complications and infections by limiting the damage to surrounding areas.
Prevention & Self-Care
Although the natural aging that causes degeneration of the spine cannot be avoided, there are some steps you can take prevent or delay the degeneration, including:
- Maintain good posture
- Stay active and exercise regularly
- Incorporate strengthening and flexibility exercises into your exercise program
- Use safe techniques when lifting or performing repetitive activities
- Maintain a healthy weight and nutritious, anti-inflammatory diet
- Don’t smoke
Staying healthy can help prevent or mitigate the symptoms of a slipped disc.