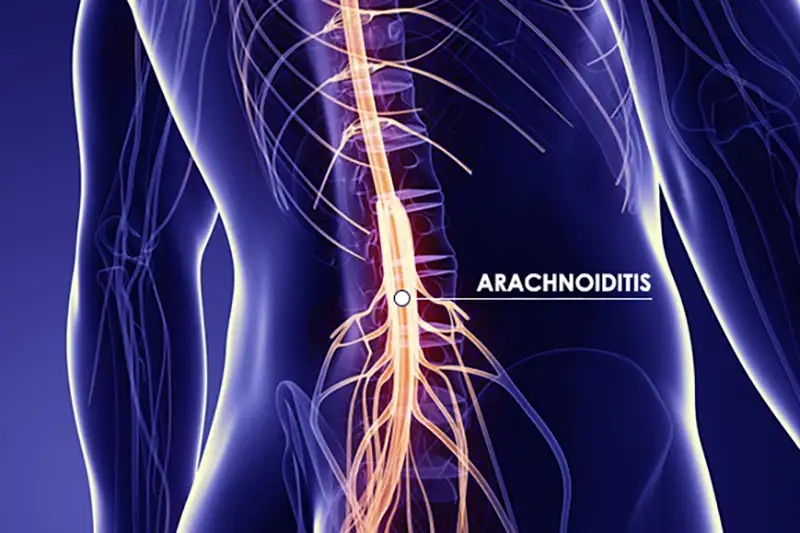
What is Arachnoiditis?
Causes of Arachnoiditis
Arachnoiditis most commonly affects adults between the ages of 40 and 60. Risk factors, such as diabetes and immunosuppressive conditions, can increase an individual’s odds of suffering from this disorder.
Some of the more common causes of arachnoiditis include:
- Spinal injury
- Bacterial or viral infections, such as meningitis
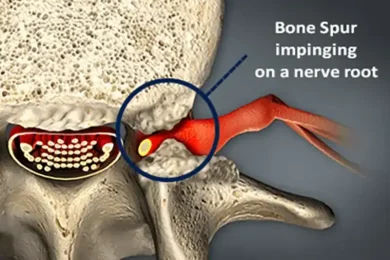
- Chronic nerve compression
- Open or fusion spinal surgery scar tissue formation
According to the National Organization for Rare Disorders, about 11,000 new cases of arachnoiditis occur in the U.S., many of which are undiagnosed. Some suggestions have also been made that epidural steroid injections and myelograms might also be to blame for cases of arachnoiditis.
Symptoms of Arachnoiditis
As with any disturbance in the spinal cord, arachnoiditis can be very painful. The most common symptom is constant pain. Some other signs of arachnoiditis include:
- Tingling, numbness, weakness in the legs
- Burning pain
- Muscle cramps
- Gait abnormalities
- Muscle spasms
- Skin sensations, such as bugs crawling on your skin
Arachnoiditis most frequently affects the lower back and lower limbs so anyone with this neurological disorder is most likely to experience these symptoms within their legs. Other signs include issues with bowel or bladder control and sexual performance.
Diagnosing Arachnoiditis
Arachnoiditis Treatment
There is no known cure for this disorder, but pain management treatment is available. Initially, non-invasive treatments such as physical therapy and pain medications may be used, although arachnoiditis does not usually respond well to conservative treatment. As these courses of treatment will not cure the condition, surgery may be another option in providing pain relief.
In cases of adhesive arachnoiditis, which causes scar tissue to form, surgery may be a viable option for pain relief. However, traditional “open” or instrumented fusion surgery should be avoided as these surgeries invariably result in the formation of new scar tissue.
Carefully targeted decompression may be effective in relieving the nerve compression caused by arachnoiditis with minimum damage to tissues, no subsequent scar formation and an enhanced long-term outcome without the use of general anesthesia.
The Bonati Spine Institute has successfully treated pain from arachnoiditis. This condition can clearly be demonstrated on an MRI. If you suffer with arachnoiditis we encourage you to submit your most recent MRI films or disc for a review by one of our surgeons to find out if you are a candidate for the Bonati Spine Procedures.