The blog is excerpted from a VeryWell Heath article by Lana Barhum updated on August 1, 2021 and medically reviewed by David Ozeri, MD.
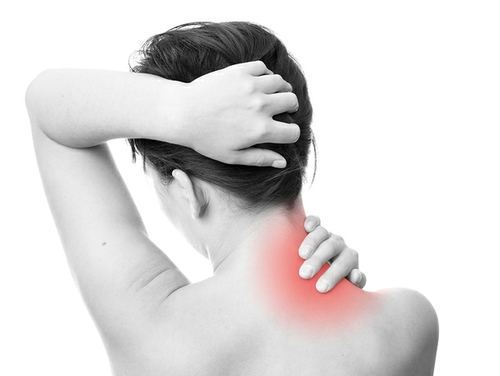
Rheumatoid arthritis (RA) is an autoimmune disorder that causes the immune system to attack its own tissues, especially the lining of joints, leading to joint damage and pain. When RA attacks the cervical spine located at the top of the spinal cord, forming the neck, it can cause neck and upper back pain. Pain in the middle or low back is not typically part of RA, but having RA may make your more prone to developing low back pain as a separate condition.
How Common Is RA Back Pain?
RA primarily affects peripheral joints—such as in the hands, feet, and knees—but the cervical spine is the second most common region that’s affected.
The spine is affected when RA progresses. In other words, inflammation in the back and spine may indicate a more advanced disease. However, the damage can be seen on X-rays as early as two years after diagnosis.
Although pain in the lumbar spine, or low back, is not commonly a part of RA, it’s associated with RA. This means that if you have RA, it’s common to also have low back pain. A 2013 study reported that up to 65.5% of people with RA may experience low back pain.
Effects of RA on the Back
RA causes inflammation in joints. The cervical spine has seven vertebrae, or bones. RA inflammation typically affects C1, also called the atlas, and C2, also called the axis. C1 and C2 are the uppermost vertebrae and they have synovial-lined joints like those of the peripheral joints.
When the immune system attacks the tissue that lines these joints it can lead to an excess of synovial fluid. This causes swelling and pain and joint erosion over time. Once C1 and C2 are affected, the inflammation can also cause pain in surrounding areas, including the upper back, shoulders, and head.
RA can also affect the facet joints of the spine. You have a pair of facet joints that run along the spine on both sides at the back of the spine. They connect to the bony bumps you feel down your back. The facet joints support the movement and flexibility of your spine. RA can cause the facet joints to become inflamed resulting in neck and/or back pain. Sometimes, chronic inflammation can cause damage to the facet joints and make the spine less stable. Instability in the spine causes a vertebra to slip out of their place where an upper vertebra slide over the lower one. This is called spondylolisthesis.
Spondylolisthesis is different from a slipped disc, or correctly named, a herniated disc. A herniated disc is usually the result of injury. C1 and C2 also are unique vertebrae that do not have discs between them. If one of the vertebrae below C1 and C2 is affected by severe inflammation, your risk for a herniated disc might be higher
Another issue that can lead to back pain in those with RA is that medications prescribed for RA, such as corticosteroids, can reduce bone mineral density as a side effect. This can lead to osteoporosis, also known as low bone mass, that increases the risk of bone fractures.
Symptoms
When RA involves the cervical spine it does not always cause early symptoms, but as it progresses pain and other symptoms may develop. Neck pain is the most common symptom and tends to be one of the earliest indications that you may have cervical spine involvement in RA.
In addition to neck pain, symptoms of RA affecting the spine include:
- Headaches
- Joint swelling and stiffness in affected parts of the back
- Loss of function and movement
- Pain in the shoulders, upper back, or base of the skull
- Stiffness in the back and neck
- Warmth around affected joints
- Tenderness in the affected areas of the back
- Pain radiating down one or both arms, indicating cervical nerve root involvement
- A crunching feeling—called crepitus—which is most notable in the neck.
Damage to facet joints from RA or other causes, such as general wear and tear, can make the spine less stable and cause vertebrae slip over one another. If this occurs in the lower spine and/or there is slipped disc, it may contribute to sciatica, or pressure on the sciatic nerve that runs along the lower back and hip.
An unstable or damaged vertebra can press on other vital parts of the body. It can also cause severe pain, deformity, and loss of height.
Symptoms of sciatica in those with low back pain can include:
- Problems with walking
- Loss of bowel or bladder function
- Loss of coordination
- Pain radiating into the legs
Diagnosis
Your healthcare provider can diagnose your neck and back pain and figure out if it is related to RA or if something else is causing it. The first thing they need to do is determine whether back pain is acute or chronic. Acute back pain tends to be caused by straining of the back with twisting, lifting something heavy, or other injury-related cause. Chronic back pain, or back pain lasting 12 weeks or longer, is usually caused by a problem in the spine or another body area.
To diagnose the source of back pain, your healthcare provider will perform a physical exam, ask questions about where it hurts and when. They may send you for X-rays and other imaging, including magnetic resonance imaging (MRI), computerized tomography (CT) scans, myelography, bone scans, and/or ultrasounds to determine damage and nerve and spinal cord involvement. If your healthcare provider thinks there is facet joint involvement, a medial branch nerve block might be done. If the pain resolves, this confirms facet joint involvement. A medial branch nerve block involves injecting anesthetic near the small medial nerves connected to a specific facet joint. More than one level is injected. This procedure is for diagnostic purposes only. If your healthcare provider thinks you need a longer pain relief treatment, a medial branch radiofrequency neurotomy (or ablation) will be done.
Find Relief from RA Linked Back Pain at the Bonati Spine Institute
Back pain is common in those with RA. The autoimmune disorder can directly attack joints of the cervical spine at the neck or the facet joints at the back of the spine, leading to inflammation and pain. It’s also common for people with RA to have coexisting low back issues that are separate from their RA. Treatments can help with pain management and/or to slow the progression of RA. If you have RA and develop chronic neck or back pain, allow our surgeons to provide a complimentary review your case to determine if you are a candidate for our exclusive Bonati Spine Procedures. The patented Bonati Spine Procedures are targeted, precision outpatient procedures performed on an incremental basis to pinpoint and eliminate the main causes of back or neck pain one level at a time. We have been able to help numerous guests suffering from RA linked back and neck pain alleviate those chronic symptoms. Simply call 844-663-0310 or complete our contact form here and a Bonati patient advocate will be happy to reach out to you directly to discuss.
Read the full VeryWell Heath article here: https://www.verywellhealth.com/rheumatoid-arthritis-back-pain-4774294