What Is Foraminal Stenosis?
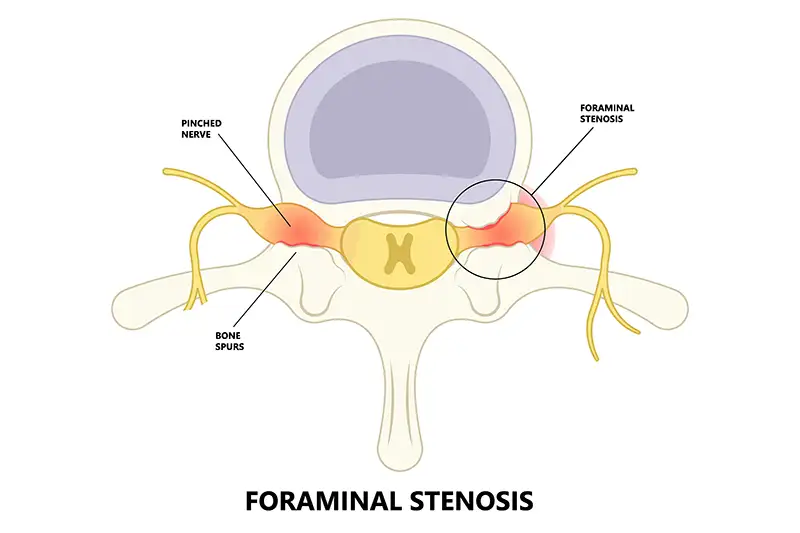
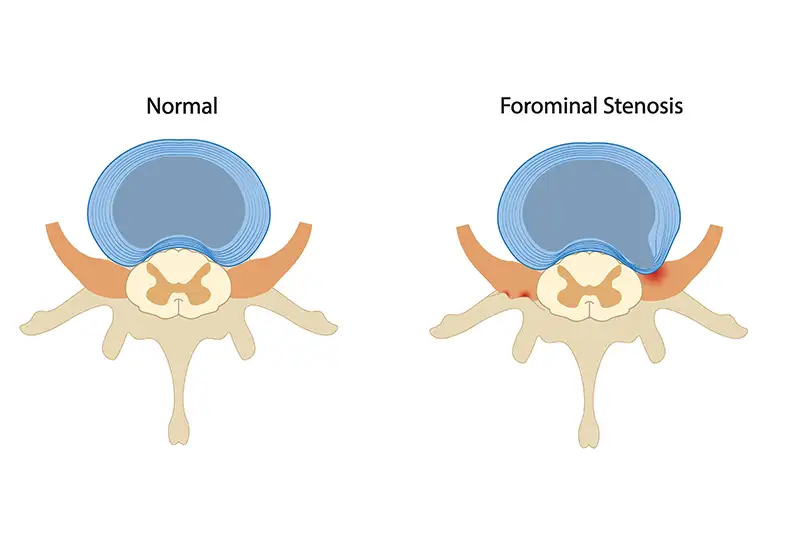
Foraminal stenosis, also known as neural foraminal narrowing, is a form of spinal stenosis in which the foramina, the small openings between vertebrae through which spinal nerve roots exit the spinal column, become narrowed and begin to compress those nerves. When a nerve root is pinched or compressed inside a narrowed foramen, it can produce significant pain, tingling, numbness, or muscle weakness along the entire pathway that the nerve serves.
Back pain affects an estimated 80 percent of Americans at some point in their lives, and foraminal stenosis is one of the more common structural causes of both acute and chronic spine pain. Your spinal column is made up of 34 bones: 24 articulated vertebrae and 10 fused vertebrae forming the sacrum and coccyx. At every level of the spine, a pair of spinal nerves exits through openings called foramina. When those openings narrow due to degeneration, injury, or other structural changes, the nerve compression results in foraminal stenosis pain.
What Causes Foraminal Stenosis?
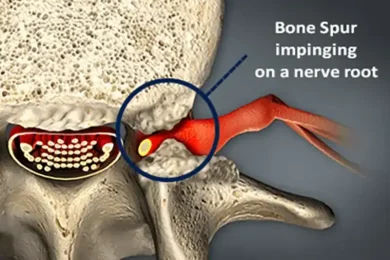
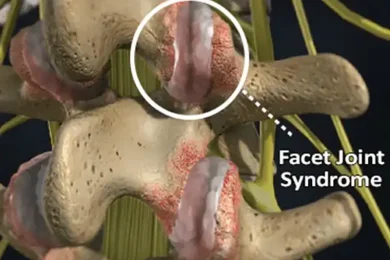
The most common cause of foraminal narrowing is the natural aging process. As the spine ages, the discs, joints, and surrounding structures gradually break down, reducing the available space for nerve roots to exit safely. However, a number of specific conditions can accelerate or directly cause this narrowing, including herniated or bulging discs, bone spurs, degenerative disc disease, spondylolisthesis, spinal arthritis, facet joint enlargement, and prior spinal injuries.
Certain risk factors can increase a person’s likelihood of developing foraminal stenosis. Genetics play a role, as some individuals are born with narrower foraminal canals. Age-related disc degeneration reduces disc height over time, shrinking the space available for nerves. Repetitive physical activity and occupational strain can accelerate wear on the spine, and excess body weight places additional load on the vertebrae and discs, speeding up the degenerative process.
In bilateral foraminal stenosis, the narrowing affects both sides of the spine rather than a single nerve root. This can cause symptoms on both sides of the body simultaneously. While foraminal narrowing can occur at any level of the spine, it is most common in the cervical (neck) and lumbar (lower back) regions, where movement and mechanical stress are greatest.
Symptoms of Foraminal Stenosis
Foraminal stenosis symptoms often develop gradually over months or even years, which is part of what makes the condition easy to dismiss in its early stages. Many patients initially attribute the discomfort to muscle soreness, a stiff neck, or the general aches of daily life. Because the foraminal canals narrow slowly, the nerve compression worsens incrementally, and symptoms tend to follow the same pattern. What begins as mild, occasional discomfort can progress into persistent, debilitating pain that significantly limits mobility and quality of life.
Because the pain and neurological symptoms of foraminal stenosis follow the pathway of the affected nerve, where you feel symptoms often depends on which level of the spine is involved. Compression in the cervical spine tends to produce symptoms in the neck, shoulders, and arms, while lumbar foraminal narrowing typically causes symptoms that radiate into the hips, buttocks, and legs. This traveling pain pattern is known as radiculopathy and is one of the hallmark signs that a spinal nerve root is being compressed.
Common symptoms of foraminal stenosis include:
- Persistent or recurring pain in the neck, upper back, or lower back
- Numbness or tingling that radiates into the arms, hands, legs, or feet
- Muscle weakness in the arms or legs, making everyday tasks more difficult
- A burning, electric, or pins and needles sensation along the nerve pathway
- Radiating pain that travels from the spine into the extremities (radiculopathy)
- Reduced grip strength or difficulty lifting objects
- Pain that worsens with prolonged sitting, standing, or certain movements
- Muscle spasms in the neck or back
Some patients experience flare-ups followed by periods of relative relief, while others deal with constant, unrelenting discomfort. In either case, the underlying structural narrowing does not resolve on its own, and symptoms will typically worsen over time without treatment. If you are experiencing sudden loss of bowel or bladder control, severe leg weakness, or extreme and rapidly worsening pain, please seek emergency medical care immediately. These can be signs of cauda equina syndrome, a serious neurological condition requiring urgent attention.
Diagnosing Foraminal Stenosis with Medical Imaging
Diagnosing neural foraminal narrowing typically begins with a thorough review of your medical history and a physical examination to assess pain levels, range of motion, and reflexes. Imaging studies including MRI, CT scan, and X-ray provide detailed information about the size and condition of the foraminal canals and surrounding structures, helping to confirm the diagnosis and identify the specific levels of the spine that are affected. The Bonati Spine Institute offers a no-obligation MRI review for patients who want expert insight into their imaging before committing to any course of treatment.
Non-Surgical Treatment for Foraminal Stenosis
When foraminal narrowing is first diagnosed, conservative measures are typically explored before surgical intervention is considered. Non-surgical approaches focus on managing pain and inflammation, improving spinal support, and slowing further degeneration. These may include over-the-counter or prescription anti-inflammatory medications, oral corticosteroids, epidural steroid injections to reduce nerve inflammation directly at the source, physical therapy to strengthen the muscles that support the spine and improve posture, chiropractic care, hot and cold therapy, and structured activity modification to reduce movements that aggravate the compressed nerve.
Because these approaches address the symptoms of nerve compression rather than the underlying structural narrowing, many patients find that relief is temporary or incomplete. Anti-inflammatory medications can ease acute flare-ups but do not stop the foraminal canal from continuing to narrow over time. Injections may provide a window of relief, but their effects typically diminish with repeated use.
If conservative treatment has not produced significant, lasting improvement after several months of consistent effort, surgical intervention is likely the most effective path forward.
The Bonati Spine Procedures: Foraminal Stenosis Surgery
When conservative treatment fails to produce meaningful improvement, the Bonati Spine Procedures offer several targeted, minimally invasive surgical options for foraminal stenosis. Unlike traditional open spine surgery, these patented procedures are performed through small incisions using specialized instruments designed to access and treat the affected area with minimal disruption to surrounding tissue. The result is less surgical trauma, reduced risk of complications, and a significantly faster recovery. Procedures are performed on an outpatient basis under conscious IV sedation with local anesthesia, eliminating the risks associated with general anesthesia and allowing patients to remain comfortable and aware throughout the process.
Specific surgical procedures used to treat foraminal stenosis at the Bonati Spine Institute include:
- Foraminotomy to enlarge the narrowed foraminal canal and create more space for the compressed nerve root to exit freely
- Laminectomy or laminotomy to decompress the spinal cord and relieve pressure on the nerve roots by removing a portion of the lamina
- Facetectomy to address joint overgrowth that is contributing to foraminal narrowing and spinal pressure
- Discectomy to remove the portion of a herniated or bulging disc that is encroaching on the foraminal space and compressing the nerve
- Facet thermal ablation to vaporize irritated nerve tissue around the facet joints and provide targeted pain relief
Our Bonati spine surgeons will review your MRI and imaging in detail, evaluate the specific levels of your spine affected, and recommend the combination of procedures best suited to your individual condition. Most patients report immediate relief as nerve pressure is released during the procedure, and many are walking out of the facility the same day. For those who have spent months or years managing foraminal stenosis pain with limited results, the Bonati approach offers a level of precision and recovery speed that traditional spine surgery simply cannot match.
Why Patients From Around The World Choose the Bonati Spine Institute in Hudson, FL
The Bonati Spine Institute performs its patented procedures on an outpatient basis using conscious IV sedation with local anesthesia, which means no general anesthesia and a significantly faster recovery than traditional open spine surgery. Patients frequently report immediate relief as nerve pressure is released during the procedure. Most are able to walk out of the facility the same day, and many return to work within days.
If you have been living with the pain of foraminal stenosis and conservative treatments have not provided lasting relief, contact the Bonati Spine Institute today.