Overview
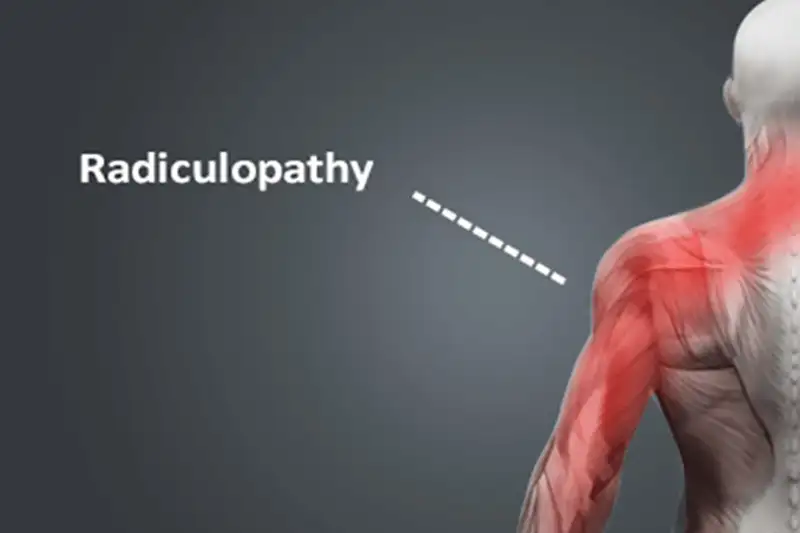
Radiculitis (radicular pain) may occur when a spinal disc presses against nerves that connect to the spinal cord. Because the spinal nerves branch out to other areas of the body, the symptoms of this nerve pressure can be felt in other places besides the location of the affected disc and nerve root. Sciatica is the most common form of radiculopathy that is caused by a pinched nerve in the lumbar spine.
Anatomy
The spinal cord acts as a highway that passes sensory information between the body and the brain. Located inside the spinal canal, it comes off the base of the brain and runs through the cervical spine and stops at the lower part of the thoracic spine, forming the central nervous system. The nerve roots come off the bottom of the cord and form a bundle called the cauda equine (horse’s tail).
The spinal cord is protected by the vertebrae that make up the spinal column. Intervertebral discs separate and cushion each vertebra and keep them from rubbing together. On the back of each vertebra are bony projections that make up the vertebral arch and spinal canal. The arch consists of two supporting pedicles and two laminae. The spinal canal contains the spinal cord, ligaments, fat, and blood vessels. A pair of spinal nerves exit the spinal cord and branch out through the body.
What is Radiculopathy?
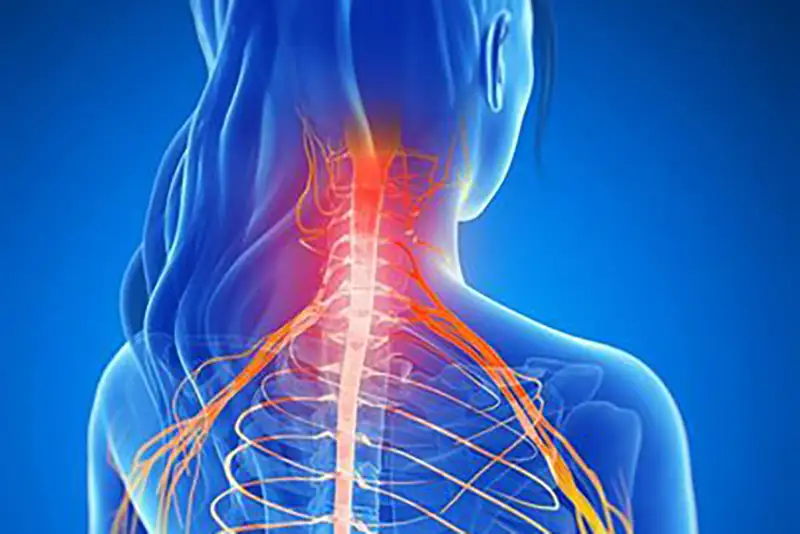
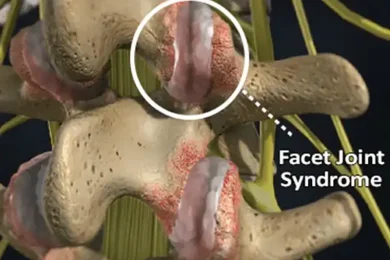
Radiculopathy is caused by compression of one or more of the nerve roots as they exit the spinal column. It can occur at any part of the spine, however, it is most commonly found in the lower back and the neck. It occurs less often in the thoracic spine.
Types of Radiculopathy
There are distinct types of radiculopathy associated with each of the three main sections of your spinal column, listed below.
Cervical Radiculopathy
The second most common type of radiculopathy, cervical radiculopathy is the clinical description of pain and/or neurological symptoms resulting from any type of condition that irritates a nerve in the cervical spine (neck). When a nerve root in the cervical spine is irritated through compression or inflammation, symptoms of pain, tingling, numbness, and/or weakness can radiate anywhere along that nerve’s pathway into the shoulder, arm, and/or hand.
Lumbar Radiculopathy
The most common type of radiculopathy, lumbar radiculopathy is caused by inflammation, compression, and/or injury to a spinal nerve root, or sciatic nerve in the low back. Causes of this type of pain, in the order of prevalence, include:
- Herniated disc with nerve compression
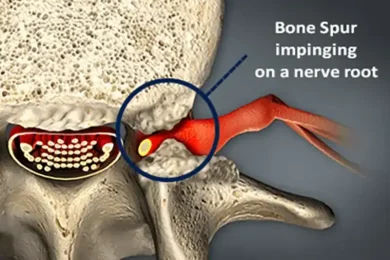
- Foraminal stenosis (narrowing of the spinal canal due to bone spurs or arthritis)
- Diabetes
- Nerve root injuries
- Scar tissue from previous spinal surgery that is affecting the nerve root
Sciatica refers to the type of pain and where it is felt. The clinical diagnosis is usually arrived at through a combination of the patient’s history (including a description of the pain) and a physical exam. Imaging studies such as MRIs and CT myelograms are used to confirm the diagnosis and will typically show the site of impingement on the nerve root.
Thoracic Radiculopathy
Compared to lumbar and cervical radiculopathy, thoracic radiculopathy is very rare. Since the thoracic spine anchors the ribs it has much less mobility and therefore, is less prone to stress as the body ages. However, patients feeling back pain shouldn’t rule out thoracic radiculopathy as the source of their pain without a diagnosis. Diagnostic tests such as an MRI, CT scan, EMG, and x-ray can pinpoint the location of the compressed nerve root.
Causes of Radiculopathy
Symptoms of Radiculopathy
Radiculopathy symptoms can range from acute to chronic and from mild to severe. The symptoms will vary, depending on the location of the compressed nerve root. There are some symptoms common to all types of radiculopathy. The affected nerves can cause hypersensitivity where the slightest touch can cause excruciating pain. If nerve damage occurs, the muscles may become weak.
The symptoms of radiculopathy can be painful and vary based on the region of the spine, or specific vertebra, affected by the condition. Those suffering from radiculopathy may experience the following signs.
- Referred pain into the upper or lower extremities often accompanies back or neck pain. Referred pain can be the initial symptom of radiculopathy caused by a compressed nerve root stemming from a ruptured disc or stenosis caused by bone spurs.
- Radicular pain is described as sharp or even shock-like pain and may be associated with certain activities or positions.
- Sensory changes are also often seen with complaints of tingling and numbness being very common.
- Motor function weakness is also seen when nerve roots are compressed from stenosis.
Lumbar:
- Lower back pain that radiates from the hips and into the legs
- Neuropathy (numbness) in the legs and feet, incontinence in severe cases
Cervical:
- Neck pain
- Weakness
- Tingling
- Neuropathy (numbness) in the neck, shoulder, and arm on one side of the body
Thoracic:
- Pain in the chest and torso (these symptoms are sometimes mistaken for shingles)
Symptoms of Radiculopathy in the Cervical Spine
Cervical radiculopathy can present acute pain, as with a traumatic ruptured disc, or can present pain of a more chronic and intermittent nature, as is seen in foraminal narrowing caused by bone spurs in the spine.
Typically, cervical radiculopathy affects the inferior nerve root at C5, C6 and C7 levels.
C5 Radiculopathy Symptoms
- Deltoid weakness
- Pain in the shoulder and the upper part of the lateral arm
- Paresthesias in the more distal part of the affected dermatome
C6 Radiculopathy Symptoms
- Biceps or brachioradialis weakness
- Hyporeflexia
- Paresthesias and frank sensory loss: more distal, and can extend into the hand
C7 Radiculopathy Symptoms
- Pain extending into the distal forearm or hand
- Root compression produces triceps weakness and a decreased triceps reflex
- Sensory loss in the hand
Symptoms of Lumbar Radiculopathy
Lumbar radiculopathy is a classic syndrome of lower lumbar nerve root compression. Symptoms include:
- Low back pain that may or may not have been associated with some sort of trauma and is commonly antecedent to the onset of leg pain by days to a few weeks.
- Motor weakness is also seen, but can be missed if dynamic testing is not done.
S1 Radiculopathy Symptoms
- Pain down the back of the leg and into the heel or foot.
- Sensory loss, usually over the lateral aspect of the foot.
- A loss of the Achilles reflex, specific to S1.
The Bonati Spine Institute encourages patients with radiculopathy to contact us to request a no-obligation MRI review or discuss your conditions with our medical professionals. Find out why The Bonati Spine Procedures are considered to be among the world’s best solutions when it comes to advanced spine surgery. Your pain from radiculopathy can become a thing of the past.
Diagnosing Radiculopathy
The diagnosis of radiculopathy begins with a complete medical history and physical examination by a physician. The doctor will inquire about the type and location of symptoms, how long they have been present, what makes them get better and worse, and what other medical problems the patient has. Knowing the exact location of the symptoms helps the doctor pinpoint the compressed nerve.
Risk Factors
Understanding the controllable risk factors for radiculopathy can help patients slow the onset of symptoms, even if they cannot prevent them completely. Although radiculopathy can be brought on by overuse, injury or trauma, poor body mechanics, poor ergonomics, and genetic factors, the most common cause is aging.
Certain risk factors can accelerate the development and progression of radiculopathy. Some risk factors include:
- Osteoarthritis and rheumatoid arthritis
- Obesity
- Poor posture
- Spinal abnormalities such as scoliosis
- Repetitive movements
Exams & Tests
Imaging tests may be ordered to help find the compressed or irritated nerve. An x-ray is often ordered first to rule out trauma, osteoarthritis, tumor, or infections as the cause of radiculopathy. Then an MRI scan may be ordered to get a look at the soft tissues around the spine including the discs, nerves, and ligaments. If the patient cannot obtain an MRI, a CT scan can be used instead. In some cases, the doctor may order an electromyogram (EMG) to determine if there is damage to the nerve.
Treatment for Radiculopathy
Conservative, non-surgical treatments can be effective for some patients. When conservative treatment is not successful, the symptoms are not resolved and quality of life is still affected, surgical intervention may be necessary.
Non-Surgical Treatment
Non-surgical treatment for the symptoms of radiculopathy may include:
- Anti-inflammatory medications
- Physical therapy
- Chiropractic care
- Epidural steroid injections
Surgical Treatment
Nerve decompression surgeries such as foraminotomy/foraminectomy, facetectomy, laminotomy/laminectomy, or discectomy may be performed to relieve the nerve pressure causing the symptoms of radiculopathy.
Prevention & Self-Care
Radiculopathy cannot be prevented, but the chances of developing it can be reduced. Maintaining good posture and a healthy weight, staying physically active, using safe techniques when lifting heavy objects, quitting smoking, and avoiding excess strain on the neck and backbone can reduce the chances of developing radiculopathy.
The Bonati Spine Institute encourages patients suffering from radiculopathy to contact us to request an MRI review or discuss your symptoms and conditions with our medical professional specialists. Find out why The Bonati Spine Institute is the world leader in advanced spine surgery.
We encourage you to contact us to request an MRI review or discussion with one of our medical professionals. Find out why The Bonati Spine Procedures are considered to be among the world’s best solutions for spine problems.