Neural Foraminal Stenosis
Understanding what neural foraminal stenosis is, its symptoms and causes, will allow you to choose the treatment option that is right for you.
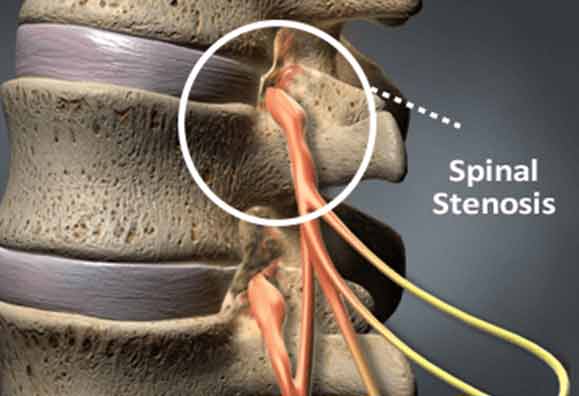
What is Neural Foraminal Stenosis?
Neural foraminal stenosis refers to compression of the spinal nerves as they leave the spinal canal. Spinal nerve roots exit through small openings between the vertebrae. When foraminal stenosis occurs, these openings (called foramina) narrow. This spinal narrowing can occur in either the lumbar spine (lower back) or the cervical spine (the neck), and can be caused by a bone spur (osteophyte) a foraminal herniated disc, or a collapse of the disc space.
Causes of Neural Foraminal Stenosis
Neural foraminal stenosis can be caused by many factors, including aging as well as underlying lifestyle-related conditions and disease.
- Congenital – in rare occurrences people are born with this condition
- Age – natural wear and tear on the spine results in disc degeneration, which causes foraminal narrowing. This is the most common cause of the condition
- Bone spurs and abnormalities – bone spurs (osteophytes) on the foramen block the pathway to the nerve roots
- Diseases – diseases such as rheumatoid arthritis, osteoarthritis, chronic meningitis, spondylolisthesis, or spinal column tumors
- Herniated disc – a disc may herniate and protrude into the foramen and compress the nerve root
- Spinal cord Injuries – trauma or repetitive motion-related injuries can cause degeneration
- Obesity – being overweight can put additional stress on the spine and cause it to deteriorate at a faster rate
Symptoms of Neural Foraminal Stenosis
The symptoms vary depending on the severity of the narrowing, the original width of the foramen, and the vulnerability of the nerves affected. The site of the narrowing will determine the location of the symptoms. Cervical foraminal stenosis affects the head, shoulders, upper back, arms, and hands. Thoracic foraminal stenosis affects the ribcage, shoulders, arms, and internal organs. Lumbar foraminal stenosis affects the lower back, buttocks, legs, and feet.
Below are some common symptoms of neural foraminal stenosis:
- Pain while walking or standing that goes away when resting
- Back pain that can be relieved in certain positions that give the nerve root more space, such as bending or flexing
- Tingling, numbness, muscle weakness, and spasms in the extremities
- Loss of control of the bladder and bowel movement, in extreme cases
- Muscle weakness in the extremities
Diagnosing Neural Foraminal Stenosis
Your doctor will ask questions about your medical history, the symptoms you are feeling, and how long you’ve had them. The physician may require a physical examination to get a clear picture of the severity of your condition and any associated risks it may pose.
In addition, you may have a neurological examination to determine the abnormalities in sensation and strengths of the compressed area. This will also be used to exclude other possible causes such as arthritis. An MRI or CT scan may be ordered to quantify the amount of narrowing of the spinal canal.
Treatment for Neural Foraminal Stenosis
Treatments recommended for neural foraminal stenosis will depend on the severity of the symptoms, whether they are acute of chronic, and if they impact your daily activities.
Non-Surgical Treatment
Patients with mild to moderate symptoms often try conservative, non-surgical treatments to relieve their pain. These treatments include:
- Over-the-counter or prescription pain medication
- Exercise to strengthen the back muscles so they can better support the spine
- Physical therapy to improve the condition of the muscles and bones
- Chiropractic treatment to align the spinal cord and relieve pressure on the nervous system
- Alternating ice and heat therapy to reduce inflammation in the nerve tissue
- Lifestyle changes such as losing weight or ceasing repetitive movements that cause degeneration
- Epidural corticosteroid injections to reduce inflammation
Surgical Treatment
In cases where chronic or severe symptoms adversely affect your day-to-day activities, and conservative treatment has yielded little or no pain relief, your physician may suggest a surgical procedure.
Traditional open back surgery and spinal fusions often require an extensive dissection of muscle tissue, several days of hospitalization, and an often painful and long recovery.
The Bonati Spine Procedures are safe and effective alternatives to traditional open spine surgery and spinal fusion. The Bonati Spine Procedures are performed on an outpatient basis, under local anesthesia and through a small incision, the patients are able to return to their daily activities within days after surgery.
Click here to see our patient’s recovery from Spinal Stenosis
